In Part 1, we looked at what 20th c. energy
healer Bill Gray had to say about healing in general, and neurological healing
in particular. We compared his view of
the lower abdomen as the master brain that produced a magnetic field with
today’s thinking about the enteric brain.
We used the phase monitor as a metaphor for the gut. Finally, we speculated about how aiding the
gut viscerally might be an avenue to improving its functioning at the energetic
level.
In Part 2, we are going to use the field effect transistor
as a metaphor for the myelin-sheathed
neuron and speculate about how supporting myelin may be an avenue to healing
damage from antidepressants.
Bill Gray on nerve
transmission
Just to remind you, although Bill Gray focused on supplying
energy to the magnetic field in the abdomen, he also worked on smoothing out
energy spasms and re-connecting broken connections in nerves throughout the
body. The goal was for energy to be
supplied smoothly everywhere along the nervous system.
If you’re not Bill Gray, how do you MacGyver a repair to
neurons that are not transmitting signal as they should?
Field effect transistors
A transistor is a device that conducts electrical
current. Think of it as a rod with
current coming in one end and going out the other. The field effect transistor (FET) was invented in 1926, but not
really used until 1947. Think of it as
a T-shape, with a second rod bumping into the first rod at a right angle. Current coming along the second rod toward
the intersection of the two rods can create a field that blocks current in the
first bar. This is how you control the
current (Wiki, encyclopedia.kids.net.au, see very helpful Youtube by engineer
Doug Peters in Sources).
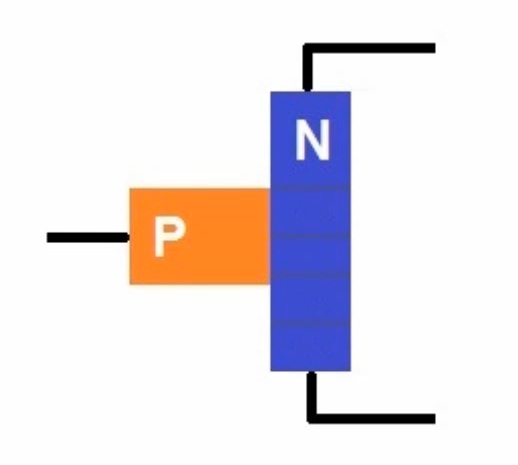 |
| FET, Source: http://www.youtube.com/watch?v=CLLcRRBph90 |
In 1959, the metal-oxide-semiconductor field-effect
transistor -- MOSFET – was
invented. It works basically the same
way, but instead of having something like a second rod interfering with the
first rod, it uses a substance (usually silicon dioxide) wrapped around the
first rod in order to create a field that allows or blocks the current. This is the transistor that is in computers
and everywhere in your life now (Wiki).
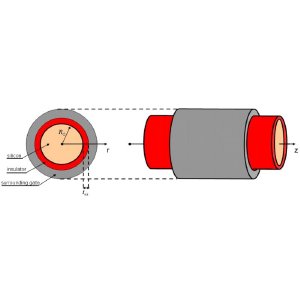 |
| MOSFET, Source: http://www.azonano.com/ |
The important thing to take from this crude description is
that you have a current going along a channel, and then you have something else
serving as a “gate.” Furthermore, the
gate cannot open the channel further; it cannot amplify the current. All it can do is close the channel partly or
all the way. It can increase resistance
to the current. In doing that, it
reduces the capacitance or capacity of the channel.
Lastly, this gate works by creating a field effect, a kind
of neutral zone, where there can be no charge.
A new perspective on
antidepressant-induced dysautonomia
Many people who stop taking antidepressants – even if they
taper off slowly – are left with clear signs of neurological
destabilization. The symptoms may be
caused by dysautonomia or dysregulation of the autonomic nervous system.
The subjective experience is that too much is happening too
fast. So, people often handle it by
trying to reduce stimulation. They stay
in their homes, and wear sunglasses and earplugs all day indoors. Think of this as trying to reduce the
current coming into a transistor at one end of that first rod. We’re trying to control the input, so
there’s less output – less sensory overload, less anxiety, etc.
This helps to some extent, but not enough. What if we have been focusing on the wrong
part of the transistor – the input – instead of on the gate? After all, if you think about it, there
really has not been an increase in input – we are still living in peacetime,
conventional neighborhoods. It *feels*
like we’re living in a war zone, but we’re not.
What would it look like to enhance the gate function instead
of vainly trying to limit input from what is already a normal level of
surrounding stimulation?
Neurons and myelin sheaths
A neuron has a lot in common with a transistor. It conducts an electrical current from one
end to the other. A myelin sheath is a
fatty casing that wraps around neurons and works in a way that is, at the
least, metaphorically like a MOSFET, and at the most, very much like a
MOSFET.
 |
| Myelin around neuron, Source: multiple-sclerosis-research.blogspot.com/ |
Myelin speeds signal transmission on a neuron, but it does
this by causing resistance to the current.
The myelin sheath segments create resistance, and decrease
capacitance. On an unmyelinated stretch
of neuron, the signal proceeds by exchanging charged ions across the membrane
(this is called the action potential).
But in a segment of neuron that is encased in a myelin sheath, the ions
are kept within the membrane (Wiki).
“As for how myelin reduces capacitance,
one first has to understand a bit about how a neuron cell membrane is
constructed and the structure of the myelin sheath. In the neuron cell
membrane, capacitance occurs because of the hydrophobic center of the plasma
membrane, which is an insulator, and the hydrophilic surfaces (both
extracellular and intracellular) that are good conductors.
Myelin, like neurons, also is
composed of cells with cell membranes constructed by a lipid bilayer with a
hydrophobic center and hydrophilic surfaces (this is common to all cells).
Myelin wraps around neurons MANY times. Each turn of myelin around the neuron
works like another capacitor connected in SERIES. This is the key concept. If
you have capacitors in series, the total capacitance remains constant while the
capacitance of each cell membrane is reduced by a factor proportional to the
number of capacitors (wraps of cell membrane). So, if there were 25 wraps of
myelin around a section of neuron, the capacitance in that location would be
1/25th of the capacitance in an area that did not have myelin.
The reason that myelin speeds the
action potential is that an action potential is NOT generated along the areas
covered by the myelin sheath. The membrane depolarization, divided among all
those layers of myelin, isn't adequate to reach the threshold potential
required to produce an action potential. So, a full action potential only
occurs at the nodes of Ranvier, which are the gaps between the myelinated
sheaths” (“Moonbear,” staff, physicsforums.com, 2008, http://www.physicsforums.com/showthread.php?t=258168).
Now, what I don’t know is whether the myelin sheath works
metaphorically like a MOSFET – both increase resistance and decrease capacitance
– or whether it has even more in common with a MOSFET. The MOSFET uses a field effect to intercede
with the current. So far, I have not
found any mention of the myelin sheath working via field effect. But, given the developing thinking about how
the brain and body operate using field effects, I wonder if it is just a matter
of time before we discover that myelin does create a field effect, and
therefore serves as a kind of gate.
So, if the lower abdomen / magnetic field / enteric brain
might work as a phase monitor, then the myelin sheath segments on a neuron may
work like a transistor, a MOSFET. This
is the kind of metaphor Bill Gray might have used to explain what was needed to
relieve “nerve energy spasms.”
Of course, the nervous system is infinitely complex, with
many different things going on. There
are a lot of mechanisms that serve as “gates” in the system. “Inhibition” and “antagonism” are basic to
the binary-ish functioning of the nervous system. So, just take this myelin-as-MOSFET as a metaphor that gives us a
constructive direction to explore.
Antidepressants and myelin
There are two questions that concern us – How is myelin
affected by taking antidepressants? And
how is myelin affected by stopping an antidepressant after taking one for
awhile? There appears to be little
research done on the first question and none done on the second question.
If you search PubMed, the biomedical journal database, for
“antidepressant myelin,” you find 156 articles since the database began, and
only 83 published in the last 26 years since Prozac came on the market.
If you search for “antidepressant serotonin,” you find
29,509 articles total, and 23,313 since Prozac.
But there are some indications that antidepressants have an
effect on myelin. Here are just a few
hints that there might be something important going on --
* Antidepressants
may cause abnormalities in myelin, http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3565193/
* Perinatal
antidepressant exposure may change myelin sheath formation,
* Antidepressants in
vitro may activate the system that produces cholesterol and fatty acids that go
into making myelin, http://www.ncbi.nlm.nih.gov/pubmed/16324787
* Antidepressants
may cause myelin growth and cell death of white blood cells in vitro,
* Antidepressants
may cause changes in myelin in rat brain,
In a 2011 study done by University of Mississippi Medical
Center and the University of California, San Francisco, rats were given an SSRI
antidepressant during the period that was the equivalent of being a human third
trimester fetus or infant. The
researchers observed behaviors that were suggestive of neurological problems
and analgous to human autism spectrum disorder (ASD) behavior. Among their findings --
Another brain abnormality common in
ASD is a thinner corpus callosum, particularly in the forward third of the
structure. Like a massive nerve-fiber bridge, the corpus callosum connects the
brain’s two halves and transmits electrical signals between them. It also plays
a key part in higher intellectual function, said Ian Paul, UMMC professor of
psychiatry and human behavior.
“This nerve fiber tract was
disrupted in the same way in these rats’ brains,” he said.
Many callosal axons in the treated
rats had abnormal or missing myelin sheathing, a coating necessary for proper
neuroconductivity.
“Without that myelin wrapping the
signal slows or doesn’t get through at all. The abnormalities in these rats
would suggest the left and right sides of their brains are not communicating
properly,” said Paul, a senior co-author on the paper (O’Brien, 2011).
So, it is reasonable to speculate that antidepressants have
an adverse effect on myelin.
Omega-3 (fish oil) and myelin
Omega-3 fatty acids are polyunsaturated essential fatty
acids. The human body doesn’t produce
them, and needs to get them from food.
There are three – EPA and DHA, which originate in algae, but market
forces have determined that we get them from the fish who eat the algae – and
ALA, which comes from seeds (Wiki).
Omega-3 has many, many functions in the human body, and it
has more than one mechanism of action.
It also has many, many functions in the nervous system. One of its functions is to build and repair
myelin (Tremblay, 2011).
There have been studies that suggested that some cultural
groups, such as Greenland Inuits and Japanese, have a diet high in Omega-3, and
have a very low incidence of multiple sclerosis, which is a disease that
involves loss of myelin. The studies
focused on the anti-inflammatory benefits of Omega-3, but it is interesing to
consider Omega-3’s pro-myelin function in light of multiple sclerosis’ loss of
myelin. http://www.ncbi.nlm.nih.gov/pubmed/7457208?dopt=Abstract
There have also been several clinical studies that show
significant benefits from mega-dose Omega-3 for severe psychological
problems. For example, in a McClean
Hospital, Harvard Medical School study, people with bipolar disorder were given 9.6 grams
of Omega-3 per day for four months.
Analysis showed “that the omega3 fatty acid patient group had a
significantly longer period of remission than the placebo group (P = .002;
Mantel-Cox). In addition, for nearly every other outcome measure, the omega3
fatty acid group performed better than the placebo group” (Stoll et al., 1999)
There have also been two recent cases of people suffering
from massive traumatic brain damage and in a coma, who recovered after
receiving mega-dose Omega-3.
In the first case of Randal McCloy, who was injured and
trapped in a mining accident in 2006, his neurosurgeon Julian Bailes, M.D.
administered 20 grams per day of “Omega-3 fish oil.” It is unclear if this was 20 g of Omega-3 or 20 grams of fish oil
which would mean less Omega-3. The
terms “Omega-3” and “fish oil” are often used interchangeably. But, Omega-3 fatty acids, are, in fact, a
component of fish oil.
“The damage to McCloy's brain was
profound, according to Bailes. Not only did it experience massive cell death,
the protective sheath around McCloy's nerve cells had been stripped during the
hours of exposure to toxic gases. That sheath, called myelin, allows brain
cells to communicate with one another.
Bailes consulted with a fish oil
expert and eventually decided that administering 20 grams a day of omega-3 fish
oil through a feeding tube might repair the myelin sheath” (Smith, 2012).
The results –
“Less than three weeks after the
mine disaster, McCloy was emerging from his coma. Three months after that, he was
walking and speaking” (Smith, 2012).
Something similar happened in the case of Bobby Ghassemi,
who was injured in a car accident in 2010, when Michael Lewis MD convinced the
family that there was no hope of spontaneous recovery and to give mega-dose Omega-3
a try based on McCloy’s dramatic recovery.
Here’s what happened –
Two weeks after beginning the
regimen, Ghassemi was emerging from his coma.
"We saw hand movements on the
left side," Peter Ghassemi said. "Around the fifth or sixth week,
there was some movement, and then his hands started moving more, the leg was
moving more."
Soon after that, Bobby began to
show signs of recognizing his family and his dog and of discerning things like
colors and numbers. Slowly, his brain was recovering, and his family ardently
believes that the high-dose fish oil is the reason why.
"His brain was still
recovering, but with (omega-3), it recovered much faster and in a shorter
amount of time," Peter Ghassemi said. "His brain was damaged, and
this was food for the brain."
Three months after his accident,
Bobby Ghassemi was well enough to attend his high school graduation (Smith,
2012).
So, it is reasonable to speculate that high-dose Omega-3 may
be beneficial for myelin health, and may contribute in that way to healing from
neurological and psychological problems.
Call for research
Research is proceeding on the use of Omega-3 for many
different neurological and psychological problems, but very little research is
being done on antidepressant-induced neurological damage in general, and no
research is being done on the effect of high-dose Omega-3 on antidepressant
damage.
I have been immersed in the online antidepressant withdrawal
support forums since 2005, and many people are taking Omega-3, but they take it
at a low to moderate dose. As far as I
know, no one has tried taking Omega-3 anywhere near the 9,000 mg dose that has
been used in some clinical neuro / psych studies.
Why is this?!
===============
Thanks to Stan for the screenshot of the field effect
transistor!
===============
Sources:
O’Brien, J.
(2011). Antidepressant linked to
developmental brain abnormalities in rodents.
http://www.ucsf.edu/news/2011/10/10827/antidepressant-linked-developmental-brain-abnormalities-rodents
Smith, S. (2012). Fish oil helped save our son. http://www.cnn.com/2012/10/19/health/fish-oil-brain-injuries/index.html
Stoll, A.L., Severus, W.E., Freeman, M.P., Rueter, S., Zboyan,
H.A., Diamond, E., Cress, K.K., & Marangell, L.B. (1999). Omega 3 fatty
acids in bipolar disorder: a preliminary double-blind, placebo-controlled
trial. Archives of General
Psychiatry, 56 (5): 407-12.
Tremblay, L. (2011).
Do Omega 3 fatty acids play a role in myelin production?
http://www.livestrong.com/article/474358-do-omega-3-fatty-acids-play-a-role-in-myelin-production/
this is a wonderful piece sheila, its all very exciting, I cant wait to read your newest and no doubt greatest essay on this topic, it certainly makes alot of sense..
ReplyDeletenever stop blogging, your a wonderful writer..i was gripped
Brilliant piece Sheila, and makes alot of sense, its all very exciting I must say and your writing is wonderful, I was gripped!!
ReplyDeleteHi, Iggster! Great to see you here! Thanks very much for the encouragement! Hopefully, energy healing and Omega-3 hold some promise for the battalions of SSRI w/d sufferers coming down the pike. I'm looking forward to seeing your ideas develop, too.
Delete